What do you do 37 times in a given workweek? If you are a fervent coffee drinker, perhaps that is how often you refill your trusty travel mug. But if you are like the physicians recently surveyed by the AMA, 37 may be the number of prior-authorization (PA) requests that you and your hardworking staffers complete each week. That is just one of the alarming results of a new survey that demonstrates the toll prior authorization is taking on patients, physicians and medical practices.
Those 37 weekly PA requests are just an average, based on a Web-based survey of 1,000 physicians administered in December. To be included in the survey physicians must have provided 20 or more hours of care each week and completed at least some PA requests during a typical practice week.
At the high end, 23 percent of respondents said they and their staff completed more than 40 prior-authorization requests in the week before taking the survey. Twenty-three percent reported they and their staff completed between 21 and 40 PA requests, while only 14 percent reported completing five or fewer.
75% say burden is high
Handling all those requests translates into a “high” or “extremely high” burden for 75 percent of physician respondents. Only 6 percent described the burden as “low” or “extremely low.” The time suck for medical practices is dreadful, with 22 percent of physicians reporting that they or their staffers spend more than 20 hours a week completing PA requests. The survey found that an average of 16.4 hours of physician and staff time each week is spent on completing PA requirements to get patients the medicines, medical services or procedures they need.
On an annual basis, that is nearly 853 hours consumed by prior-authorization tasks. The time burden is so great that about one-third of physicians have staff members who work exclusively on prior-authorization duties.
Ninety percent of surveyed physicians reported that the PA process delays patient access to necessary care.
Forty-four percent of doctors say PA requests “often or always” hold up care.
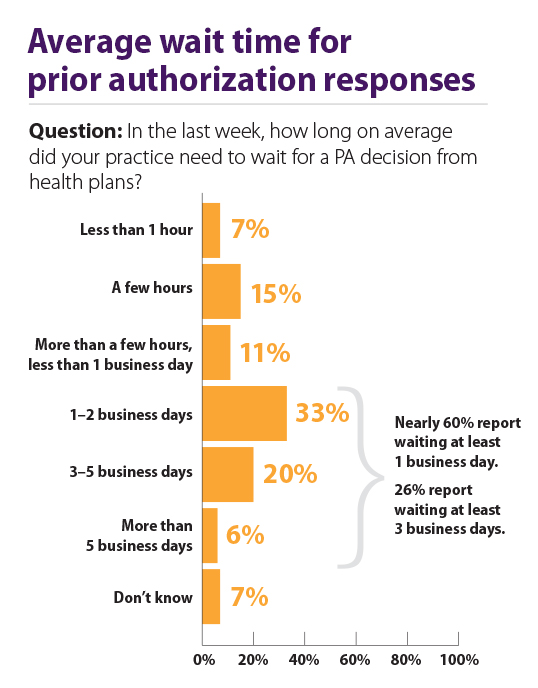
And those delays are often lengthy, with 26 percent of physicians saying that, in the prior week, they waited three business days or more on average to receive PA decisions from health plans.
Fax modems and phone trees
Another maddening aspect of the prior-authorization rigmarole is how disconnected the process is from the rest of the clinical workflow and modern technology. In our computer age, the most commonly reported ways to complete PA requests remain the fax machine and the telephone. That is a draining burden for practices, as these time-consuming, antiquated methods interrupt the practice workflow and pull physicians and their staff away from patient care.
Moreover, the prior-authorization exercise has acquired the flavor of a Sisyphean task. Eighty percent of physicians report they are sometimes, often or always required to repeat PA requests for prescriptions when the patient has already been stabilized on a treatment for a chronic condition.
The PA process exemplifies the kind of clerical work that now consumes about half of physicians’ time in the office, while less than 30 percent of the day is spent on direct clinical care. These growing diversions from patient care serve as physicians’ biggest source of professional dissatisfaction.
Clear path offered
Last week, the AMA and a coalition of 16 other organizations representing physicians, medical groups, hospitals, pharmacists and patients issued a comprehensive set of 21 principles designed to dramatically reshape the prior-authorization process. Among other things, the coalition calls for an end to repeated PA requirements for patients already stabilized on a medication for a chronic condition. The coalition also seeks industry-wide standardization of the PA process through electronic transactions that are incorporated into electronic health record systems. The 21 principles encompass clinical validity, continuity of care, transparency and fairness, timely access and administrative efficiency, and alternatives and exemptions.
The AMA offers a variety of resources to help physicians address prior-authorization issues.
In 2016, the AMA House of Delegates adopted in-depth policy on standardization and simplification of prior authorization. Several states have already passed legislation to protect patients from overly burdensome utilization-management requirements, with Delaware and Ohio among the most recent.