In the shift toward value-based care, physicians are getting paid by their practices in a variety of ways. Learn six key things about payment trends that physicians should know and see how you stack up.
A new AMA report sheds light on physician payment methods as it examines data on non-solo physicians from 2014. Based on a nationally representative survey of post-residency physicians who provided at least 20 hours of patient care per week, the report highlighted six trends:
- Slightly more than one-half of physicians (51 percent) reported being paid by multiple methods. Thirty percent received compensation through two methods, and 14.4 percent received payment through a combination of three methods.
- Salary and productivity-based payment were the most common payment methods. Sixty-one percent said they received a salary, and 53.5 percent reported receiving productivity-based payment.
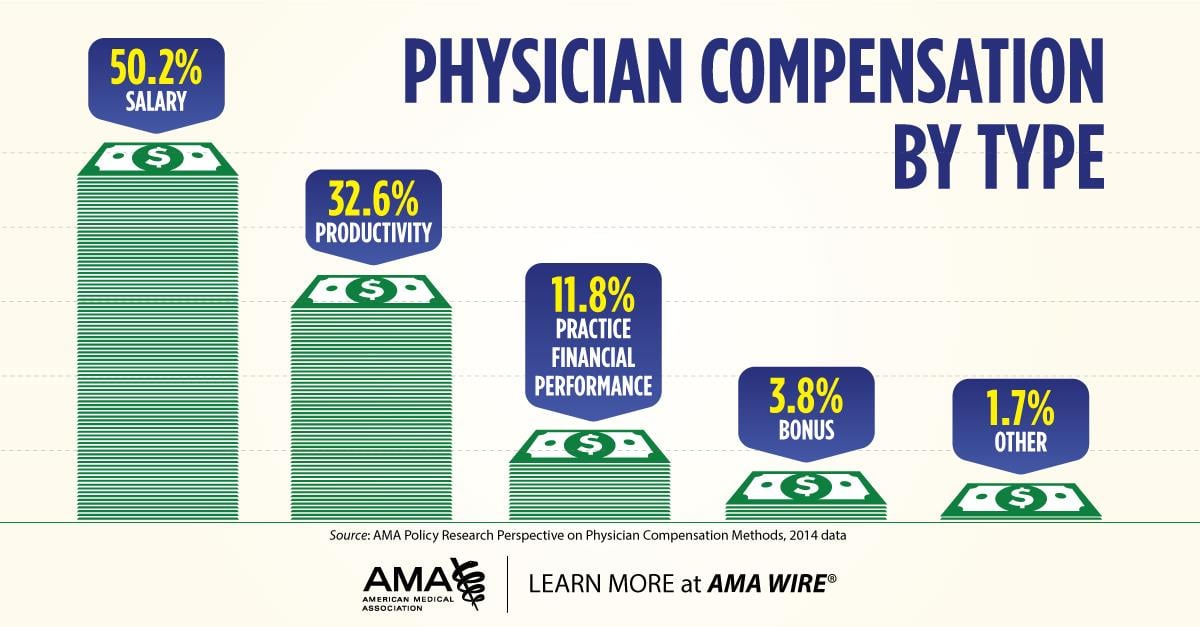
- On average, one-half of physicians’ total compensation was earned from salary. Also on average, about one-third of payment was based on productivity, 11.8 percent was based on practice financial performance, and about 5.5 percent was from a bonus or other methods. However, these shares varied greatly depending on the physician’s practice ownership status.
- Being employed didn’t necessarily mean a salary. Twenty-three percent of employed physicians didn’t receive salaried payments at all. Productivity was a common payment method, with almost one-half receiving at least some pay based on productivity and 13.8 percent receiving payment exclusively based on their productivity.
- Outside of group practice, salary was more often a key factor than inside group practice. In group practices, 42.4 percent of physicians in a single-specialty practice and 52.9 percent in a multi-specialty practice received more than one-half of their compensation from salary. For physicians not in a group practice (for example, physicians who worked in a faculty practice plan, medical school, or who were employed by a hospital), more than three-quarters relied on salary for more than one-half of their compensation.
- Physician payment methods vary widely across specialties. The percentage of physicians who were exclusively salaried ranged from 9.4 percent of surgical specialists to 47.9 percent of psychiatrists.
The report shows that the structure of physician payment appears to have changed little between 2012—the last AMA study of this kind—and 2014. The largest changes in these years came in the use of productivity-based pay (from 50.5 percent of physicians who received that method in 2012 to 53.5 percent in 2014) and bonuses (from 27.1 percent in 2012 to 30.5 percent in 2014).
New payment models
According to the AMA’s recent joint study with the RAND Corporation, physicians are attempting to transition to new payment models but need help successfully managing and responding to the many quality programs and payer metrics so they can ensure their long-term sustainability. In addition, despite the continued focus on alternative payment models, this report indicates that productivity-based pay is still an important factor in physician compensation.
The findings from the AMA-RAND study dovetail with the AMA’s Professional Satisfaction and Practice Sustainability initiative, which is paving the way for physicians to successfully navigate the health care environment in sustainable practices that can result in improved outcomes for patients and greater professional satisfaction for physicians and their health care teams.
Meanwhile, the AMA is focusing advocacy efforts on reducing the tsunami of regulatory penalties and working to make it easier for physicians to adopt new payment models. That includes urging Congress to pause Stage 3 of the meaningful use electronic health record incentive program and bringing physicians’ concerns with the program to the forefront.
In addition, the legislation that repealed the sustainable growth rate (SGR) formula includes financial support for physicians who want to participate in new care delivery and payment models. Beginning in 2019, physicians who choose to develop and participate in new models of care will receive bonus payments from Medicare. Read more about how the SGR repeal law supports new payment models.