If you’re preparing for the United States Medical Licensing Examination® (USMLE®) Step 2 exam, you might want to know which questions are most often missed by those taking the practice test. Check out this example from Kaplan Medical, and view an expert video explanation of the answer. Also check out all posts in this series.
This month’s stumper
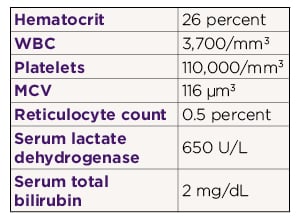
A 54-year-old lawyer presents to the emergency department with diarrhea for the past two months. He has associated fatigue, shortness of breath and weight loss. He has lost approximately 10 pounds over the last few months, during which time the symptoms have worsened. He has no related medical history and does not smoke or drink. He takes no medications. On examination his blood pressure is 115/75 mm Hg and his pulse is 108 per minute. His skin is pale. Neurologic examination reveals loss of vibration sense, spasticity and a positive Babinski sign. Laboratory studies show:
Which of the following is the most likely diagnosis? A. Alcoholic liver disease
B. Folate deficiency
C. Hemolytic anemia
D. Myelodysplastic syndrome
E. Vitamin B12 deficiency
The correct answer is E.
Kaplan Medical explains why
Macrocytosis (MCV >110 fL), diarrhea and neurologic symptoms strongly suggest vitamin B12 deficiency. Diarrhea from celiac sprue, bacterial overgrowth or pancreatic insufficiency can be seen with vitamin B12 deficiency because these are malabsorptive syndromes. The vitamin is absorbed in the terminal ileum; it is facilitated by intrinsic factor. When B12 deficiency develops in the presence of chronic atrophic gastritis, it is known as pernicious anemia.
Neurologic symptoms of vitamin B12 deficiency are due to the effect on the posterior and lateral columns of the spinal cord (subacute combined degeneration). Physical findings include symmetrical paresthesia with loss of vibratory and position sense. Neurologic findings may precede anemia and usually take longer to resolve with treatment. Obtaining a serum B12 level is the standard diagnostic test. In patients with borderline levels, serum methylmalonic acid levels may be checked. The Schilling test historically was used to help determine the cause of the B12 deficiency; however, it has now been largely replaced by measuring for antiparietal cell antibodies. The presence of antiparietal cell antibodies is indicative of pernicious anemia.
Why the other answers are wrong
Read these explanations to understand the important rationale for why each answer is incorrect.
Choice A: There is no history suggestive of alcoholic liver disease. The presence of target cells is seen in liver disease but is a nonspecific finding. Mechanisms for alcohol-related macrocytic anemia include the direct toxic effects of alcohol on bone marrow, coexisting with folate deficiency due to malnutrition, liver disease and iron deficiency. It takes many months to deplete the body’s stores of B12 because the vitamin is stored in the liver.
Choice B: In contrast to vitamin B12 deficiency, folate deficiency can develop relatively quickly. On top of this, folate deficiency does not give neurological signs or symptoms. Causes include nutritional deficiency, alcoholism, malabsorption, pregnancy, chronic hemolytic states and the administration of drugs that interfere with folate metabolism (for example, trimethoprim and methotrexate).
Choice C: Hemolytic anemia is suggested by the high LDH and bilirubin; however, the low reticulocyte count indicates a vitamin B12 deficiency.
Choice D: Although anemia, leukopenia and thrombocytopenia may suggest myelodysplastic syndrome, the degree of macrocytosis, the diarrhea and the neurologic symptoms are suggestive of a vitamin B12 deficiency. In addition, hypersegmented neutrophils may be seen. The diagnosis is confirmed with bone marrow biopsy.
One tip to remember
Deficiency of vitamin B12 results in macrocytic anemia and neurologic deficits. This is extremely important to remember because folate deficiency does not cause neurologic deficits.
For more prep questions on USMLE Steps 1 and 2, view other posts in this series.