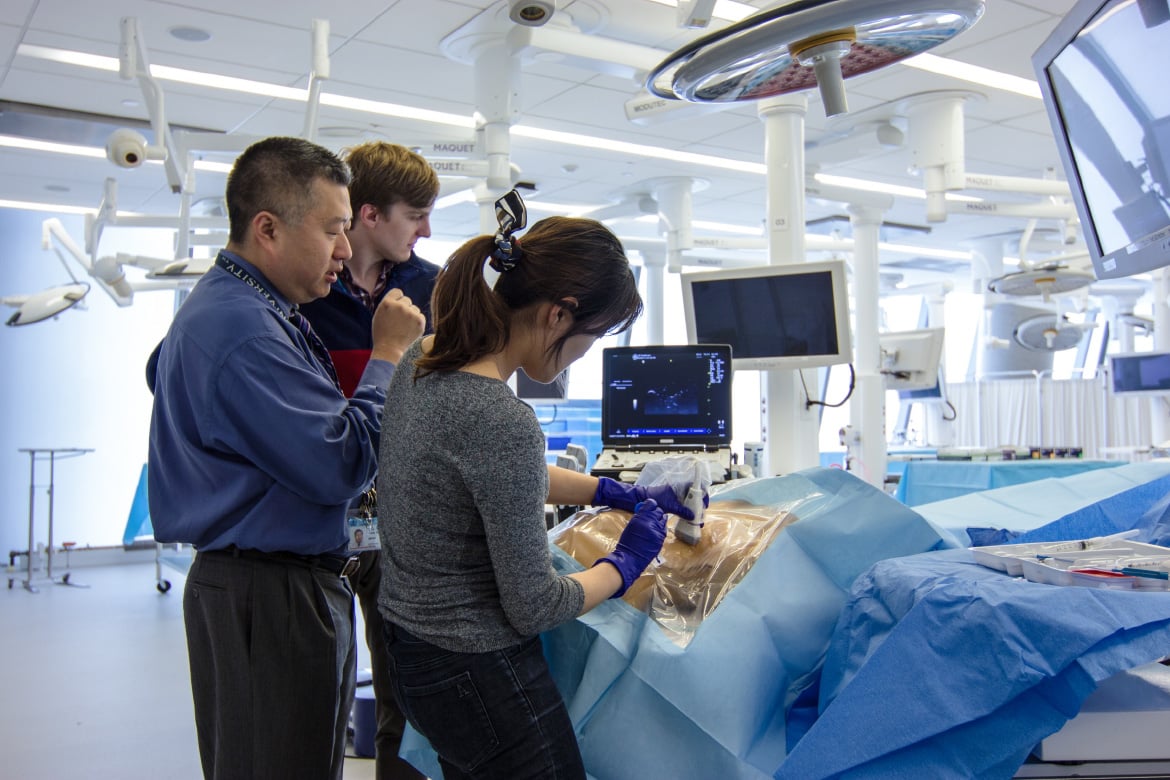
What medical students know is only as good as how they apply it. Bridging the gap is key to ensuring a successful transition from medical school to residency.
“One of the things that is lacking overall [in medical education] is a way to successfully help students translate their book knowledge to action and taking care of patients,” said Rachel Gordon, MD, MPH, associate professor of medicine and epidemiology at Columbia University Irving Medical Center. “During medical school, you are either in the classroom or you’re on the wards, but sometimes you need a combination of the two.”
To give students that combination, Dr. Gordon has created a month-long blended learning course at Columbia that aims to prepare fourth-year medical students for the next level. Offered in the spring prior to graduation, the Ready for Residency program uses interactive classroom-based learning sessions. There are digital sessions with virtual patients and hands-on skills and simulation training to create residents who are confident and familiar with the situations they will encounter on day one.
Leaving lectures behind
The prior program—Back to the Classroom—was lecture-centric. Considering where students are in their training, Dr. Gordon was challenged to find a fresh approach.
“A lot of these boot camp [or residency-training programs] use lecture still,” she said. “Who wants to sit there listening to a lecture when you need to learn how to function as a physician? There’s a limited effectiveness of lecture at the end of the year when [students] are all anxious to hit the wards.”
Ready for Residency is required of all fourth-year Columbia medical students and takes a multifaceted approach to teaching to the 13 Core Entrustable Professional Activities for Entering Residency laid out by the Association of American Medical Colleges. That approach includes active learning sessions each morning, weekly simulation and skills sessions and daily virtual rounds in an online portal.
At the outset of the course, students are separated into small teams mixed by specialty. These teams work together throughout all phases of the course.
During virtual sessions in what Dr. Gordon calls the “e-hospital,” student teams attend to one main patient per week. They work together to order tests, prescribe medications and diagnose and treat conditions. Dr. Gordon and her colleagues then offer students granular, specific feedback on tasks that they will be expected to do on their first day as residents, such as writing orders.
“As the course progresses, I see their teamwork improve as they work together more cohesively and effectively, ,” Dr. Gordon says. “They form tight bonds.”
Cementing lessons with simulation
Throughout the course, student teams partake in six simulations of emergent situations, developed by Julia Iyasere, MD, associate medical director of Columbia's simulation center. The scenarios focus on teamwork and team roles and often serve to reinforce lessons that students have encountered online or during their classroom sessions.
Dr. Gordon pointed to lessons students learn about acute coronary syndrome (ACS) as an example of how the simulations can be effective.
“When faced in a simulation with a patient with crushing chest pain about to have cardiac arrest, the ability to actually get the EKG and to give the person an aspirin in a timely fashion—that’s stuff that ... you can answer on a multiple choice test, but your ability to actually do it is very different,” she said.
“When they first start out, they aren’t necessarily able to treat ACS very smoothly and effectively. By the end, they can,” Dr. Gordon said.